What is BRCA?
Every human has both a BRCA1 and BRCA2 gene, which help to suppress tumor formation and growth. When the genes function properly, they help repair damaged DNA in human cells, which can lead to cancer. Occasionally, however, a mutation exists in the BRCA1 or BRCA2 gene, which substantially increases a person’s risk of developing cancer.
A large cohort study of 6,036 women with BRCA1 mutations and 3,820 women with BRCA2 mutations (Kuchenbaecker et al, 2017) found that the lifetime risk of breast cancer is approximately 72% (BRCA1) or 69% (BRCA2), compared to an average lifetime risk of 12% in the general population. Lifetime ovarian cancer risk also increases to 44% (BRCA1) and 17% (BRCA2), compared to a lifetime risk of 1.3% in the general population.
For more information, please see the National Cancer Institute’s Fact Sheet on BRCA.
When should BRCA carriers be screened for cancer?
The National Comprehensive Cancer Network (NCCN) provides screening guidelines for women with a known BRCA mutation (updated July 30, 2018).
- Starting at age 18:
- Breast awareness including breast self-exams
- Starting at age 25:
- Clinical breast exam every 6-12 months
- Age 25-29:
- Annual breast MRI with contrast
- Age 30-75:
- Annual mammogram and breast MRI with contrast
- Age 30-75:
- Transvaginal ultrasound and CA-125 blood test for ovarian cancer (at clinician discretion)
- Age > 75:
- Individual management of cancer risks
For more information, please see the National Comprehensive Cancer Network’s Clinical Guidelines.
What surgical options are available?
Prophylactic surgery may be an option for female BRCA mutation carriers to reduce their risk of developing cancer:
- Prophylactic bilateral mastectomy (PBM) is the surgical removal of both breasts
- Prophylactic bilateral salpingo-oophorectomy (PBSO) is the surgical removal of both ovaries and fallopian tubes
There are some additional decisions regarding breast reconstruction following a PBM. A surgical oncologist or general surgeon typically performs the mastectomy, and a plastic surgeon typically performs reconstruction surgery.
- No reconstruction
- Reconstruction with saline or silicone implants
- Reconstruction with a woman’s own fat cells (called DIEP or TRAM flap)
- Nipple-sparing mastectomy
- Under or over the muscle implants
NCCN also provides recommendations for women regarding surgery to reduce cancer risk:
- Discuss prophylactic bilateral mastectomy (PBM) with your physician and genetic counselor.
- Recommend prophylactic bilateral salpingo-oophorectomy (PBSO) after completion of child bearing, and by age 35-40 (for BRCA1 carriers) or age 40-45 (for BRCA2 carriers).
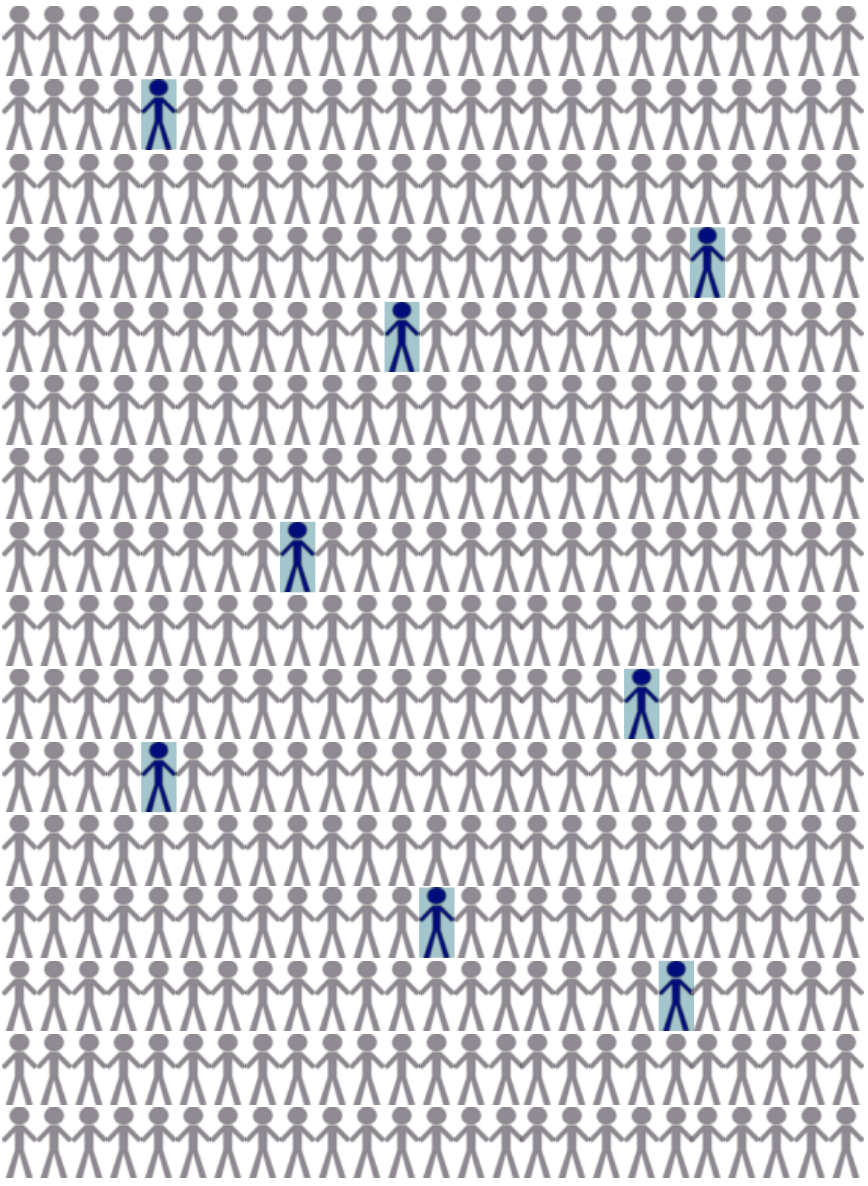
How common are BRCA mutations?
Approximately 1 in 400 people living in the United States carry a BRCA1 or BRCA2 mutation. Among some populations, the rate is much higher. For those of Ashkenazi Jewish (AJ) descent, approximately 1 in 50 carry a BRCA1 or BRCA2 mutation. Among the AJ population, the 3 most common mutations are known as founder mutations, which are: c.68_69delAG (BRCA1), c.5266dupC (BRCA1), c.5946delT (BRCA2).

How is BRCA inherited?
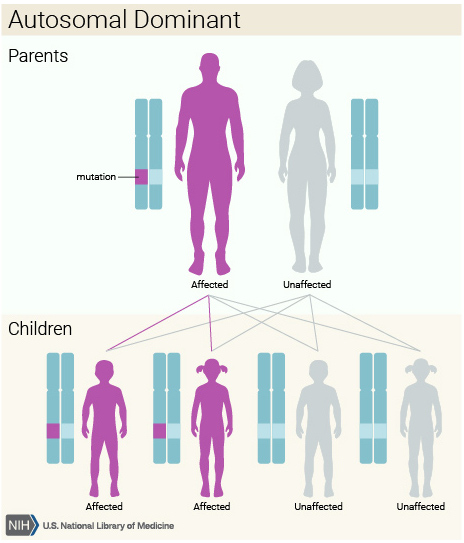
BRCA genetic mutations are known as germline mutations, which means they are inherited from either a mother or father. Every child inherits 2 copies of every gene (1 from each parent), except for genes on the sex chromosomes. BRCA mutations are inherited in an autosomal dominant pattern, which means that a person needs only 1 mutated copy of the gene to be affected. If a mother carries a BRCA mutation, there is a 50% chance her child will inherit the mutation; the same is true if a father is a BRCA mutation carrier. This is different from recessive genetic disorders, such as Tay-Sachs, where 2 mutated copies (from both parents) are needed for a child to be affected.
Only 1 parent needs to have genetic mutation
(e.g., Huntington’s disease, BRCA)
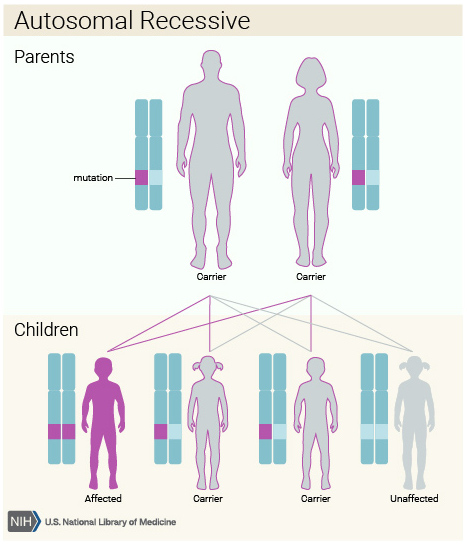
Both parents need to have genetic mutation
(e.g., Cystic fibrosis, Tay-Sachs)
What is the difference between BRCA1 and BRCA2?
BRCA1 and BRCA2 are completely different genes, with BRCA1 located on chromosome 17 and BRCA2 located on chromosome 13. Both genes are inherited from parents in an autosomal dominant manner. It is possible (although rare) to carry mutations in both BRCA1 and BRCA2 genes.
The risk of breast and ovarian cancer also differs between the genes. A large cohort study of 6,036 women with BRCA1 mutations and 3,820 women with BRCA2 mutations (Kuchenbaecker et al, 2017) found that the lifetime risk of breast cancer is approximately 72% (BRCA1) or 69% (BRCA2), compared to an average lifetime risk of 12% in the general population. Lifetime ovarian cancer risk also increases to 44% (BRCA1) and 17% (BRCA2), compared to a lifetime risk of 1.3% in the general population.